NEWS - JANUARY and FEBRUARY 2019
DIRECT BOOKING OF PHYSIOS, etc.
Millions to get fast support to overcome back pain, thanks to NHS Long-Term Plan
23 February 2019 ... 1 page
Tens of thousands of people have been helped to overcome back pain, arthritis and other muscle, bone and joint conditions without going to hospital, thanks to additional specialist care at local GP surgeries – with millions more set to benefit over the coming years as the NHS delivers on its Long Term Plan.
Millions to get fast support to overcome back pain, thanks to NHS Long-Term Plan
23 February 2019 ... 1 page
Tens of thousands of people have been helped to overcome back pain, arthritis and other muscle, bone and joint conditions without going to hospital, thanks to additional specialist care at local GP surgeries – with millions more set to benefit over the coming years as the NHS delivers on its Long Term Plan.
HEALTHWATCH ENGLAND CHAIR
Sir Robert Francis has been appointed as Chair of Healthwatch England for 3 years from 01 October 2018.
Healthwatch England is a Committee of Care Quality Commission (CQC), and is chaired by a non-executive director of the CQC.
Sir Robert’s appointment as a CQC Non-Executive Director, which was due to end on 30 June 2020, has been extended to align with this appointment.
The appointment will involve a time commitment of 2 days per week and remuneration will be at a rate of £30,000 per annum for both roles.
This appointment is made in accordance with the Cabinet Office Code of Governance for Public Appointments. The regulation of public appointments against the requirements of this Code is carried out by the Commissioner for Public Appointments. In accordance with the Code, there is a requirement for appointees’ political activity (if any declared) to be made public.
Sir Robert has not declared any political activity.
Sir Robert Francis has been appointed as Chair of Healthwatch England for 3 years from 01 October 2018.
Healthwatch England is a Committee of Care Quality Commission (CQC), and is chaired by a non-executive director of the CQC.
Sir Robert’s appointment as a CQC Non-Executive Director, which was due to end on 30 June 2020, has been extended to align with this appointment.
The appointment will involve a time commitment of 2 days per week and remuneration will be at a rate of £30,000 per annum for both roles.
This appointment is made in accordance with the Cabinet Office Code of Governance for Public Appointments. The regulation of public appointments against the requirements of this Code is carried out by the Commissioner for Public Appointments. In accordance with the Code, there is a requirement for appointees’ political activity (if any declared) to be made public.
Sir Robert has not declared any political activity.
NHS CLOSE FIRST; CONSULT AFTER
Article originally appeared on Lincolnshire Reporter.
The ‘temporary closures’ issue still rumbles on in the NHS. 30 months have elapsed since overnight services were withdrawn at the hospital in Grantham and local politicians are becoming restive.
Two years ago, the Independent Reconfiguration Panel looked at the case and urged the parties to work together towards a solution based on the Lincolnshire-wide plan – then part of the local STP.
It is now suggested that a public consultation will emerge that will cover the future of the local hospital. However, the real issue is that the NHS has a loophole whereby it can in certain circumstances close first and consult after – but only on a temporary basis.
Is this case stretching the concept of ‘temporary’ a bit far?
Article originally appeared on Lincolnshire Reporter.
The ‘temporary closures’ issue still rumbles on in the NHS. 30 months have elapsed since overnight services were withdrawn at the hospital in Grantham and local politicians are becoming restive.
Two years ago, the Independent Reconfiguration Panel looked at the case and urged the parties to work together towards a solution based on the Lincolnshire-wide plan – then part of the local STP.
It is now suggested that a public consultation will emerge that will cover the future of the local hospital. However, the real issue is that the NHS has a loophole whereby it can in certain circumstances close first and consult after – but only on a temporary basis.
Is this case stretching the concept of ‘temporary’ a bit far?
HEALTH SELECT COMMITTEE CHAIR
February 22, 2019 by Rhion Jones ... 2 pages
If Dr Sarah Wollaston loses the Health Select Committee Chair, we may lose a Parliamentary champion of consultation
February 22, 2019 by Rhion Jones ... 2 pages
If Dr Sarah Wollaston loses the Health Select Committee Chair, we may lose a Parliamentary champion of consultation
|
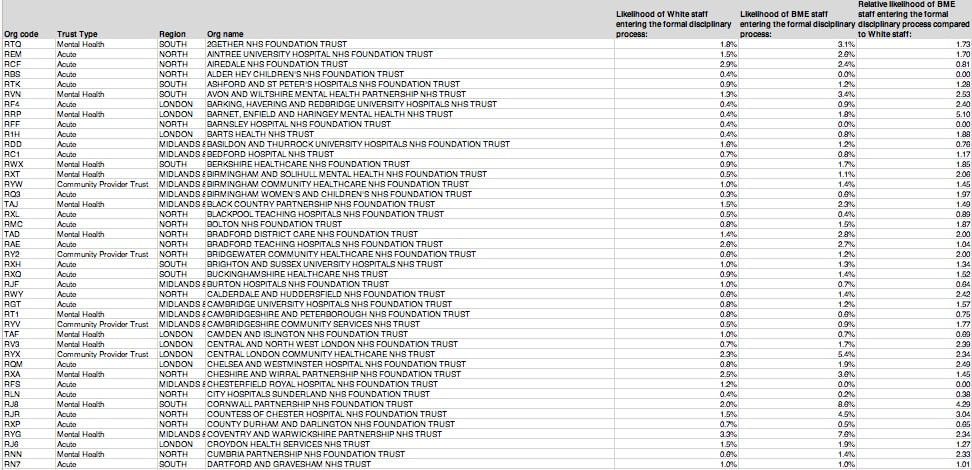
RACE AND EQUALITY BY TRUST
Excel Spreadsheet Organisation Code . Trust Type . Region . Organisation Name . Likelihood of White staff entering the formal disciplinary process . Likelihood of BME staff entering the formal disciplinary process . Relative likelihood of BME staff entering the formal disciplinary process compared to White staff. |
|
NHS WORKFORCE RACE EQUALITY STANDARD
2018 Data Analysis Report for his NHS Trusts ... 48 pages The WRES was introduced in 2015 to reveal and thereby help close the gaps in workplace inequalities between black and minority ethnic (BME) and white staff working in the NHS. Getting this right is critical; evidence shows that a motivated, included and valued workforce helps deliver high quality patient care, increased patient satisfaction and better patient safety – it also leads to more innovative and efficient organisations. |
DIGITALISATION - ALL LLOYD GEORGE RECORDS
GPs face huge task to digitise all Lloyd George records by 2022
Details of the contract published last week by NHS England say that £20m in funding to support practices with subject access requests (SARs) for patient records will stop in 2022 because 'the digitalisation of Lloyd George paper records [will be] completed' by that time.
This involves scanning notes into a PDF file for each patient. Practices are then expected to upload the PDF documents to their electronic patient records system ‘one by one’ - a process that takes ‘maybe a few minutes’ per file.
This process alone could generate hundreds of hours of work for an average-sized practice with 8,500 patients - five minutes per patient would mean 708 hours of work - more than 90 full working days. Across around 7,000 practices in England, this would add up to around 5m hours' work.
GPs face huge task to digitise all Lloyd George records by 2022
Details of the contract published last week by NHS England say that £20m in funding to support practices with subject access requests (SARs) for patient records will stop in 2022 because 'the digitalisation of Lloyd George paper records [will be] completed' by that time.
This involves scanning notes into a PDF file for each patient. Practices are then expected to upload the PDF documents to their electronic patient records system ‘one by one’ - a process that takes ‘maybe a few minutes’ per file.
This process alone could generate hundreds of hours of work for an average-sized practice with 8,500 patients - five minutes per patient would mean 708 hours of work - more than 90 full working days. Across around 7,000 practices in England, this would add up to around 5m hours' work.
NHS LONG TERM PLAN - PRIMARY CARE
According to the latest issue of PCC Insight, the new Long Term Plan finally makes good on NHS England’s pledge to reverse the decline of general practice with new funding and a new GP contract, but it also comes with conditions. Central to the success of the strategy is the ability of primary care to organise in networks and for the wider health economy to form integrated care systems – both in short order.
We hear from a former Director of Primary Care, a leading lawyer and PCC’s Chief Executive, Helen Northall, about the implications of the plan and its prospects.
We also hear from a procurement expert about the skills primary care networks will need to acquire to grow and thrive as more of the “new” money is routed through networks, and from PCC adviser Charlotte Goodson about the contracting issues faced by dispensing practices.
https://www.pcc-cic.org.uk/sites/default/files/articles/attachments/pcc_insight_feb_2019_web.pdf
According to the latest issue of PCC Insight, the new Long Term Plan finally makes good on NHS England’s pledge to reverse the decline of general practice with new funding and a new GP contract, but it also comes with conditions. Central to the success of the strategy is the ability of primary care to organise in networks and for the wider health economy to form integrated care systems – both in short order.
We hear from a former Director of Primary Care, a leading lawyer and PCC’s Chief Executive, Helen Northall, about the implications of the plan and its prospects.
We also hear from a procurement expert about the skills primary care networks will need to acquire to grow and thrive as more of the “new” money is routed through networks, and from PCC adviser Charlotte Goodson about the contracting issues faced by dispensing practices.
https://www.pcc-cic.org.uk/sites/default/files/articles/attachments/pcc_insight_feb_2019_web.pdf
SPECIFIC DIGITAL IMPROVEMENTS - PRIMARY CARE
5.10 NHS England and GPC England have agreed eight specific improvements, backed by agreed contract changes, in areas where it is realistic to make early progress, given available functionality:
(i) All patients will have the right to online and video consultation by April 2021;
(ii) All patients will have online access to their full record, including the ability to add their own information, as the default position from April 2020, with new registrants having full online access to prospective data from April 2019, subject to existing safeguards for vulnerable groups and third party confidentiality and system functionality;
(iii) All Practices will be offering and promoting electronic ordering of repeat prescriptions and using electronic repeat dispensing for all patients for whom it is clinically appropriate, as a default from April 2019;
(iv) All Practices will ensure at least 25% of appointments are available for online booking by July 2019. This is staging post towards a shared ambition that all patients should have the maximum possible access to online appointment booking. NHS England will launch a public campaign in 19/20 to raise awareness of the ability to book appointments online. Subject to systems capability, where patients wish, and as part of concluding the NHS 111 call, NHS 111 could book into these appointments on their behalf where that is appropriate, rather than requiring patients to do so in a separate process;
(v) Whilst a `practice leaflet remains important, to recognise the changing habits of patients, all Practices will need - by April 2020 - to have an up-to-date and informative online presence, with key information being available as standardised metadata for other platforms to use (for example the Access to Service Information (A2SI) Directory of Services Standard);
(vi) All Practices will be giving all patients access online to correspondence by April 2020, as the system moves to digital by default (with patients required to opt-out rather than in);
(vii) By April 2020, Practices will no longer use facsimile machines for either NHS or patient communications; and
(viii) From October 2019, Practices will register a Practice email address with MHRA CAS alert system and monitor the email account to act on CAS alerts where appropriate; notify the MHRA if the email address changes to ensure MHRA distribution list is updated; and register a mobile phone number (or several) to MHRA CAS to be used only as an emergency back up to email for text alerts when email systems are down.
---- and -----
5.19 This agreement reaffirms our commitment that primary medical care will always remain a fully comprehensive NHS service, free at the point of use. And so from 2019 it will no longer be legal for any NHS GP provider – either directly or via proxy - to advertise or host private, paid-for GP services that fall within the scope of NHS-funded primary medical services. NHS England will consult on expanding this specific ban on the provision of paid-for GP services to other providers of mainly NHS services.
https://www.england.nhs.uk/wp-content/uploads/2019/01/gp-contract-2019.pdf
5.10 NHS England and GPC England have agreed eight specific improvements, backed by agreed contract changes, in areas where it is realistic to make early progress, given available functionality:
(i) All patients will have the right to online and video consultation by April 2021;
(ii) All patients will have online access to their full record, including the ability to add their own information, as the default position from April 2020, with new registrants having full online access to prospective data from April 2019, subject to existing safeguards for vulnerable groups and third party confidentiality and system functionality;
(iii) All Practices will be offering and promoting electronic ordering of repeat prescriptions and using electronic repeat dispensing for all patients for whom it is clinically appropriate, as a default from April 2019;
(iv) All Practices will ensure at least 25% of appointments are available for online booking by July 2019. This is staging post towards a shared ambition that all patients should have the maximum possible access to online appointment booking. NHS England will launch a public campaign in 19/20 to raise awareness of the ability to book appointments online. Subject to systems capability, where patients wish, and as part of concluding the NHS 111 call, NHS 111 could book into these appointments on their behalf where that is appropriate, rather than requiring patients to do so in a separate process;
(v) Whilst a `practice leaflet remains important, to recognise the changing habits of patients, all Practices will need - by April 2020 - to have an up-to-date and informative online presence, with key information being available as standardised metadata for other platforms to use (for example the Access to Service Information (A2SI) Directory of Services Standard);
(vi) All Practices will be giving all patients access online to correspondence by April 2020, as the system moves to digital by default (with patients required to opt-out rather than in);
(vii) By April 2020, Practices will no longer use facsimile machines for either NHS or patient communications; and
(viii) From October 2019, Practices will register a Practice email address with MHRA CAS alert system and monitor the email account to act on CAS alerts where appropriate; notify the MHRA if the email address changes to ensure MHRA distribution list is updated; and register a mobile phone number (or several) to MHRA CAS to be used only as an emergency back up to email for text alerts when email systems are down.
---- and -----
5.19 This agreement reaffirms our commitment that primary medical care will always remain a fully comprehensive NHS service, free at the point of use. And so from 2019 it will no longer be legal for any NHS GP provider – either directly or via proxy - to advertise or host private, paid-for GP services that fall within the scope of NHS-funded primary medical services. NHS England will consult on expanding this specific ban on the provision of paid-for GP services to other providers of mainly NHS services.
https://www.england.nhs.uk/wp-content/uploads/2019/01/gp-contract-2019.pdf
NHS 111 AND THE GP
Source: GP Contract 2019/20
Source: GP Contract 2019/20
- NHS 111 will begin direct booking into practice appointments.
- Practices will be expected to make one appointment per 3,000 patients available each day for this.
- NHS 111 will only book the appointment after triage.
SOCIAL PRESCRIBING
An army of advisers will be recruited to help patients live fitter, healthier lives and combat anxiety, loneliness and depression under plans to ramp up social prescribing set to be launched by NHS England this week.
Around half of GP appointments are not directly related to medical conditions, according to experts.
Growing evidence shows that referrals to community services such as exercise or art classes, history groups and even ballroom dancing can boost health and wellbeing more than dishing out pills or other treatments.
Now NHS England plans to recruit 1,000 social prescribing ‘link workers’ as part of the NHS Long Term Plan. The link workers will be able to give people time to talk about what matters to them and support them to find suitable activities that are a better alternative to medication as part of a step change in the provision of ‘personalised care’.
The blueprint for Universal Personalised Care, which will also free up GPs to deal with patients who really need them, is due to approved by the NHS England Board later this week.
By 2023-24, social prescribers will be handling around 900,000 patient appointments a year.
Social Prescribing is an important component of the NHS comprehensive model of Personalised Care
https://www.england.nhs.uk/personalisedcare/comprehensive-model-of-personalised-care/
An army of advisers will be recruited to help patients live fitter, healthier lives and combat anxiety, loneliness and depression under plans to ramp up social prescribing set to be launched by NHS England this week.
Around half of GP appointments are not directly related to medical conditions, according to experts.
Growing evidence shows that referrals to community services such as exercise or art classes, history groups and even ballroom dancing can boost health and wellbeing more than dishing out pills or other treatments.
Now NHS England plans to recruit 1,000 social prescribing ‘link workers’ as part of the NHS Long Term Plan. The link workers will be able to give people time to talk about what matters to them and support them to find suitable activities that are a better alternative to medication as part of a step change in the provision of ‘personalised care’.
The blueprint for Universal Personalised Care, which will also free up GPs to deal with patients who really need them, is due to approved by the NHS England Board later this week.
By 2023-24, social prescribers will be handling around 900,000 patient appointments a year.
Social Prescribing is an important component of the NHS comprehensive model of Personalised Care
https://www.england.nhs.uk/personalisedcare/comprehensive-model-of-personalised-care/
|
PATIENT AND COMMUNITY ENGAGEMENT INDICATOR
(Compliance with Statutory Guidance on Patient and Public Participation in Commissioning Health and Care). 2018/2019 CCG Improvement and Assessment Framework. Guidance for CCGs 22 pages |
|
GUIDE - NHS CONSTITUTION, PATIENTS' RIGHTS, ETC.
158 pages Information about the rights and pledges in the NHS Constitution and what these mean for NHS patients and staff. |
|
SHOCK CANCELLATION OF BIRTHING CENTRE MEETING - HAPIA Press Release
04 January, 2019 ... 1 page A high level meeting with Prof Nick Harding, Chair of the Sandwell and West Birmingham CCG (SBCCG), planned for December 21st to discuss the future of the Halcyon Birthing Centre, was cancelled at the last minute by the CCG, because they objected to local health campaigners attending the meeting. The meeting was set up to challenge the CCG’s decision to close the unique Halcyon birthing centre, without public consultation. It was to be attended by national public involvement adviser Malcolm Alexander, and local maternity care campaigners, but local NHS leaders refused to attend if the women campaigners were present. |
|
REVIEW OF CCGs
A Review of the role and costs of Clinical Commissioning Groups, published by the National Audit Office Key Facts . Summary . The NHS Commissioning Landscape . The role and running costs of Clinical Commissioning Groups . Measurements of Clinical Commissioning Groups' performance . The future role of CCGs in a changing NHS landscape . Our review approach |
GPs - AMOUNT PER PATIENT
GP practices received £152.04 per patient in 2017/18, official data reveal - an increase of just 0.4% compared with the previous year.
GP practices received £152.04 per patient in 2017/18, official data reveal - an increase of just 0.4% compared with the previous year.