NEWS - MAY 2015
|
GENDER IDENTITY
23 pages This Report is a response to the ‘Escalation of Advice’ from Healthwatch England in respect of lack of access to gender identity services. This escalation requires NHS England to instigate an initial investigation into the issues raised and to identify whether further investigation is necessary. The investigation has been carried out by the Director of Commissioning (Corporate).
|
MERGING OMBUDSMEN?
The Queen’s Speech includes plans to merge the Health Ombudsman, Parliamentary Ombudsman, Local Government Ombudsman and potentially the Housing Ombudsman.
This would be a “simplified, improved and more accessible final tier of redress for customers of public services who have complained and who do not feel satisfied by how their complaint has been handled.”
It will also include the “opportunity to improve public services by identifying where problems are occurring and informing the creation and development of effective responses.”
A consultation on this proposal will end on 16th June.
The Queen’s Speech includes plans to merge the Health Ombudsman, Parliamentary Ombudsman, Local Government Ombudsman and potentially the Housing Ombudsman.
This would be a “simplified, improved and more accessible final tier of redress for customers of public services who have complained and who do not feel satisfied by how their complaint has been handled.”
It will also include the “opportunity to improve public services by identifying where problems are occurring and informing the creation and development of effective responses.”
A consultation on this proposal will end on 16th June.
GPs SPEND FIFTH OF CONSULTATION TIME ON NON-HEALTH PROBLEMS
A very general practice ... How much time do GPs spend on issues other than health?
22 pages
A very general practice ... How much time do GPs spend on issues other than health?
22 pages
|
GPs are spending nearly a fifth of their consultation time dealing with non-medical issues at a cost of nearly £400 million, according to a new report from charity Citizens Advice.
According to the study, ‘A very general practice’, GPs spend 19% of their time dealing with personal relationship problems, housing and unemployment concerns or work-related issues. It also reveals that three quarters of GPs say that the proportion of time they spend dealing with non-health issues as part of consultations has increased over the past year. The report comes after former RCGP chair Professor Clare Gerada said she had referred more people to food banks than A&E in one week! |
At the same time, NHS England are encouraging greater integration between social and health care, having given approval to funding ‘social prescribing’ pilot schemes.
GP leaders said that patients’ needs extend beyond ‘bio-medical’ health care, but this should not place greater burdens on GPs.
The charity surveyed 1,000 GPs in February this year on the effect of non-health problems on their workload.
The main findings included:
GP leaders said that patients’ needs extend beyond ‘bio-medical’ health care, but this should not place greater burdens on GPs.
The charity surveyed 1,000 GPs in February this year on the effect of non-health problems on their workload.
The main findings included:
- 80% report that dealing with non-health queries results in decreased time available to treat other patients’ health issues
- 64% report that non-health queries from patients increase the stress of their job
- 46% report that non-health issues raised during consultations contribute to increased costs to the practice and to the NHS
- 49% say these conversations help them better understand the communities in which they work
- 92% report that their patients had raised issues about personal relationship problems with them in the last month
NEW MINISTERS JOIN DH IN RESHUFFLE
12 May 2015
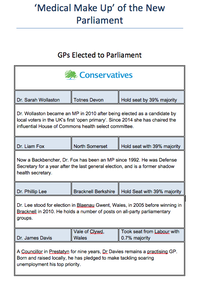
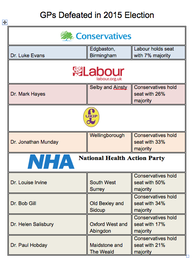
David Cameron has appointed two new Health Ministers in his Government reshuffle, following the reappointment of Jeremy Hunt as Health Secretary.
Alistair Burt is the new Minister of State at the Department of Health, while Ben Gummer has been appointed Parliamentary Under Secretary of State.
Election was an opposition whip and member of the Conservatives’ Shadow Team for the Department
Communities and Local Government.
In 1992, he was made Parliamentary Under Secretary of state for the Department of Social Security, and was
promoted to Minister of State three years later.
He first entered Parliament in 1982 for Bury North, but lost his seat in the 1997 Labour landslide. Before going
into politics he worked as a solicitor.
Writing on his website in March, Mr Burt said he was “totally reliant on the NHS, as neither I nor my family have
private health insurance”.
On the role of the private sector in the NHS, he said: “The very small element of private sector involvement in the
NHS will continue under any future government.” “The NHS has always involved a mixture [of public and private
provision]. I will continue to support the best healthcare being provided for constituents, whoever provides it.”
written a book about the Black Death. Mr Gummer ran on a platform to keep services at Ipswich Hospital,
and his website claims credit for having “successfully brought heart and other specialist services” to the hospital.
His father is the former Conservative environment secretary John Gummer.
Mr Hunt was reappointed as Health Secretary yesterday. Dan Poulter has stood down as a Health Minister
12 May 2015
David Cameron has appointed two new Health Ministers in his Government reshuffle, following the reappointment of Jeremy Hunt as Health Secretary.
Alistair Burt is the new Minister of State at the Department of Health, while Ben Gummer has been appointed Parliamentary Under Secretary of State.
- Mr Burt, who steps into the position occupied by Norman Lamb in the last Government, is the MP for North East Bedfordshire.
Election was an opposition whip and member of the Conservatives’ Shadow Team for the Department
Communities and Local Government.
In 1992, he was made Parliamentary Under Secretary of state for the Department of Social Security, and was
promoted to Minister of State three years later.
He first entered Parliament in 1982 for Bury North, but lost his seat in the 1997 Labour landslide. Before going
into politics he worked as a solicitor.
Writing on his website in March, Mr Burt said he was “totally reliant on the NHS, as neither I nor my family have
private health insurance”.
On the role of the private sector in the NHS, he said: “The very small element of private sector involvement in the
NHS will continue under any future government.” “The NHS has always involved a mixture [of public and private
provision]. I will continue to support the best healthcare being provided for constituents, whoever provides it.”
- Mr Gummer is the MP for Ipswich, and in the last Government served as Parliamentary Private Secretary to Education Secretary, Nicky Morgan.
written a book about the Black Death. Mr Gummer ran on a platform to keep services at Ipswich Hospital,
and his website claims credit for having “successfully brought heart and other specialist services” to the hospital.
His father is the former Conservative environment secretary John Gummer.
Mr Hunt was reappointed as Health Secretary yesterday. Dan Poulter has stood down as a Health Minister
|
GENERAL ELECTION 2015 - THE HEALTH AND CARE DEBATE
The debate from Tuesday 21 April, now available to watch online Click here, on the tile or on the image to view (allow it a few seconds to commence) The speakers were:
|
NHS CONTRACTING
Legal news ... Visit our blog for the latest news about legal issues affecting clinical commissioning.
Guide to the Health and Social Care Act ... Download our guide to the Health and Social Care Act.
Our health lawyers have analysed the Act to explain what has changed and what this means for commissioners, providers, local authorities and regulators.
Visit our Health Broadcast Centre for videos that are relevant to the health sector, including interviews with key decision makers working in health organisations.
Introduction to contracts ... Back to the full list of short guides
Contracting and CCGs
CCGs are responsible for commissioning many NHS services. While standard contracts will need to be used for most services, it is still important to understand how a contract is formed, tailored and performance managed.
CCGs must also be mindful of requirements to adhere to procurement legislation and policy. Further details in respect of procurement are set out in our separate briefing paper entitled Introduction to procurement and competition. CCGs also need to consider their consultation obligations when commissioning services.
Main features of contract formation The following features are essential to the formation of any contract:
This means that NHS contracts are not legally binding and so are not enforceable in the courts. While parties to an NHS contract are obliged to perform their duties and obligations under that contract, if there is a dispute either party can only refer the matter to the Secretary of State, for NHS dispute resolution.
CCGs are "health service bodies". This means that contracts between a CCG and another health service body are NHS contracts.
CCGs should note that foundation trusts are not "health service bodies", so any contracts with foundation trusts will be legally binding.
Key contractual clauses Certain key contractual clauses will be present in almost any contract. They include:
Legal news ... Visit our blog for the latest news about legal issues affecting clinical commissioning.
Guide to the Health and Social Care Act ... Download our guide to the Health and Social Care Act.
Our health lawyers have analysed the Act to explain what has changed and what this means for commissioners, providers, local authorities and regulators.
Visit our Health Broadcast Centre for videos that are relevant to the health sector, including interviews with key decision makers working in health organisations.
Introduction to contracts ... Back to the full list of short guides
Contracting and CCGs
CCGs are responsible for commissioning many NHS services. While standard contracts will need to be used for most services, it is still important to understand how a contract is formed, tailored and performance managed.
CCGs must also be mindful of requirements to adhere to procurement legislation and policy. Further details in respect of procurement are set out in our separate briefing paper entitled Introduction to procurement and competition. CCGs also need to consider their consultation obligations when commissioning services.
Main features of contract formation The following features are essential to the formation of any contract:
- Offer and acceptance – these criteria will almost always be satisfied where there is a written contract, providing the terms are sufficiently certain
- Consideration – something must be paid or provided in return for the provision of the goods or services
- Intention to create legal relations – this is usually assumed in a commercial context (though note comments below about NHS contracts)
This means that NHS contracts are not legally binding and so are not enforceable in the courts. While parties to an NHS contract are obliged to perform their duties and obligations under that contract, if there is a dispute either party can only refer the matter to the Secretary of State, for NHS dispute resolution.
CCGs are "health service bodies". This means that contracts between a CCG and another health service body are NHS contracts.
CCGs should note that foundation trusts are not "health service bodies", so any contracts with foundation trusts will be legally binding.
Key contractual clauses Certain key contractual clauses will be present in almost any contract. They include:
- Duration – How long will the contract last? Should either party have the power to extend it or terminate it early?
- Services/goods to be provided under the contract – What services/goods are to be provided and by when? Where will they be provided? Will the provider need to sub-contract any service provision?
- Payment – What is the price for the services and how is it to be calculated and paid?
- Performance monitoring – Are there to be agreed performance indicators or milestones? What will happen if they are not achieved?
- Exclusion and limitation of liability – Are there to be any exclusions or limitations of liability? Note that there are statutory restrictions on the extent to which liability can be excluded or limited.
- Termination provisions – whether, and in what circumstances, the contract can be terminated by a party. Usually this would include provision allowing for termination for certain breaches of contract.
CHOICE AND COMPETITION IN THE NHS
1. Letter to David Bennett, Chief Executive, MONITOR - from Malcolm Alexander, Chair, HAPIA - 04 April 2015
2. Response from Tom Grimes, Head of Enquiries, Complaints and Whistleblowing, MONITOR - Email, 20 April 2015
1. Letter to David Bennett, Chief Executive, MONITOR - from Malcolm Alexander, Chair, HAPIA - 04 April 2015
2. Response from Tom Grimes, Head of Enquiries, Complaints and Whistleblowing, MONITOR - Email, 20 April 2015
Ruth Marsden, HAPIA NORTH talking on BBC Radio on Monday, 13 April 2015 re. International Recruitment of Nurses.
The talk commences at 01:37:02 on the recording scale.
The talk commences at 01:37:02 on the recording scale.
LAUNCH OF NEW WAY OF WORKING FOR CQC
Letter from David Behan, Chief Executive, CQC - dated 01 April 2015
Today (1 April), we confirm our new way of monitoring, inspecting and rating care services with the formal introduction of some key changes that will make sure the public will have: greater clarity of what to expect from care providers better protection from poor care better information to support choice about the quality of local care services, including ratings of services that must be displayed prominently. The key changes include: new fundamental standards of quality and safety, read more here. introduction of our special measures regime (where services found to be providing particularly poor care are closely monitored and offered extra support to help them improve within set timescales) our new enforcement powers requirement to display ratings.
All of this ultimately strengthens how we deliver our purpose – to make sure health and social care services provide people with safe, effective, compassionate, high quality care and to encourage services to improve.
You can read more about these changes on our website: http://www.cqc.org.uk/whatwedo
Today’s launch marks the culmination of a transformation in how we monitor, inspect and regulate services and follows an extensive period of co-production, consultation, testing and development with the public, providers and other organisations with an interest in our work.
Thank you to everyone who has provided feedback and helped us to get to this point. This is a significant moment, though we recognise the need to continuously improve the way we work and we hope that you will continue to provide feedback and support us to do so.
Yours sincerely, David Behan, Chief Executive
Letter from David Behan, Chief Executive, CQC - dated 01 April 2015
Today (1 April), we confirm our new way of monitoring, inspecting and rating care services with the formal introduction of some key changes that will make sure the public will have: greater clarity of what to expect from care providers better protection from poor care better information to support choice about the quality of local care services, including ratings of services that must be displayed prominently. The key changes include: new fundamental standards of quality and safety, read more here. introduction of our special measures regime (where services found to be providing particularly poor care are closely monitored and offered extra support to help them improve within set timescales) our new enforcement powers requirement to display ratings.
All of this ultimately strengthens how we deliver our purpose – to make sure health and social care services provide people with safe, effective, compassionate, high quality care and to encourage services to improve.
You can read more about these changes on our website: http://www.cqc.org.uk/whatwedo
Today’s launch marks the culmination of a transformation in how we monitor, inspect and regulate services and follows an extensive period of co-production, consultation, testing and development with the public, providers and other organisations with an interest in our work.
Thank you to everyone who has provided feedback and helped us to get to this point. This is a significant moment, though we recognise the need to continuously improve the way we work and we hope that you will continue to provide feedback and support us to do so.
Yours sincerely, David Behan, Chief Executive
DETAILS OF PRIMARY CARE CONTROL SHIFT
The Clinical Commissioning Groups taking on full control of GP services in their area this week will be responsible for performance managing poor practices and approving practice mergers. However, NHS England will continue to have responsibility for complaints management, according to the delegation agreement it sent to CCGs. This comes in spite of guidelines issued by NHS England last year stating that this responsibility would be passed onto CCGs.
Sixty-four CCGs have been approved to take on fully delegated commissioning of GP services in 2015-16. Several group leaders previously said they were concerned about the lack of time they had to prepare to take on co-commissioning responsibilities.
CCGs were issued their delegation Agreement just two weeks before they were due to take on additional powers. It is understood that they were given only one week to sign and return the Agreement, but this was pushed back by two days following concerns being raised by some groups.
The delegation Agreement is near final confirmation of the responsibilities that will pass to the CCGs. It states that CCGs will make “decisions in relation to the management of poorly performing GP practices and including, without limitation, decisions and liaison with the [Care Quality Commission] where the CQC has reported non-compliance with standards”. This will exclude any decision relating to performers lists or individual GPs, which NHS England will continue to have responsibility for.
CCGs will be responsible for making decisions on local GP incentive schemes, “including the design of such schemes”, and on the establishment and closure of GP practices in their area, including the approval of practice mergers. They will also make decisions surrounding enhanced services, “discretionary” payments and about commissioning urgent care for out of area registered patients. However, the Agreement states that “functions in relation to complaints management” about practices or GPs will be retained for NHS England. This is a change since previous guidance. It is understood some had raised concerns with NHS England about the practical implications of moving complaints handling, as well as the risks involved in GPs’ conflict of interest.
The Agreement does state, however, that NHS England could ask CCGs to carry out some elements of processing complaints in the future.
The Clinical Commissioning Groups taking on full control of GP services in their area this week will be responsible for performance managing poor practices and approving practice mergers. However, NHS England will continue to have responsibility for complaints management, according to the delegation agreement it sent to CCGs. This comes in spite of guidelines issued by NHS England last year stating that this responsibility would be passed onto CCGs.
Sixty-four CCGs have been approved to take on fully delegated commissioning of GP services in 2015-16. Several group leaders previously said they were concerned about the lack of time they had to prepare to take on co-commissioning responsibilities.
CCGs were issued their delegation Agreement just two weeks before they were due to take on additional powers. It is understood that they were given only one week to sign and return the Agreement, but this was pushed back by two days following concerns being raised by some groups.
The delegation Agreement is near final confirmation of the responsibilities that will pass to the CCGs. It states that CCGs will make “decisions in relation to the management of poorly performing GP practices and including, without limitation, decisions and liaison with the [Care Quality Commission] where the CQC has reported non-compliance with standards”. This will exclude any decision relating to performers lists or individual GPs, which NHS England will continue to have responsibility for.
CCGs will be responsible for making decisions on local GP incentive schemes, “including the design of such schemes”, and on the establishment and closure of GP practices in their area, including the approval of practice mergers. They will also make decisions surrounding enhanced services, “discretionary” payments and about commissioning urgent care for out of area registered patients. However, the Agreement states that “functions in relation to complaints management” about practices or GPs will be retained for NHS England. This is a change since previous guidance. It is understood some had raised concerns with NHS England about the practical implications of moving complaints handling, as well as the risks involved in GPs’ conflict of interest.
The Agreement does state, however, that NHS England could ask CCGs to carry out some elements of processing complaints in the future.
|
LHW - HOW IS IT DOING?
By: Helen Gilburt ... 55 pages Phoebe Dunn Catherine Foot This report was commissioned by the Department of Health to examine the progress that had been made in the first 18-21 months of local Healthwatch and to identify the positive steps that could be taken across the system to enable a high-performing and effective local Healthwatch network. |
HEALTHWATCH ROUND-UP - March 2015 - The LGA
Our grant-funded programme of support directly to Healthwatch commissioners and for Healthwatch Health and Wellbeing Board (HWB) representatives has drawn to completion as of March 31st 2015. The LGA will still provide support to all member authorities who have concern in meeting their statutory duties for Healthwatch through our regional teams and we will still provide liaison and advice at a national policy level and communicate any messages through when necessary. We will also continue to work with local Healthwatch HWB representatives through our Care and Health Improvement Programme over the coming year.
If you are continuing to commission local Healthwatch in your area then please make sure you are signed up to the Knowledge Hub where you can access 3 years of archived discussion and support material. We have also kept a Healthwatch page as part of the LGA si with up-to-date documents for those new to Healthwatch commissioning.
Local Healthwatch: Progress and Promise' – As you know, the Department of Health commissioned the King's Fund to look at the impact and effectiveness of local Healthwatch since they were set up in April 2013. The report has now been published and you can read it on GOV.UK. I've also put a copy up on the Knowledge Hub.
One of the findings in the report is around the important role local authority commissioners play in the development and overall effectiveness of their local Healthwatch and there are some recommendations about how this might be developed going forward. Colleagues at DH have asked me to pass on their thanks to everyone who took part.
We hope you have found the support and materials from the LGA over the past few years helpful and encourage you all to stay connected to offer peer support and share learning through network meetings and on the Knowledge Hub.
John Tench
Healthwatch Adviser
john.tench@local.gov.uk
07786 541890
Our grant-funded programme of support directly to Healthwatch commissioners and for Healthwatch Health and Wellbeing Board (HWB) representatives has drawn to completion as of March 31st 2015. The LGA will still provide support to all member authorities who have concern in meeting their statutory duties for Healthwatch through our regional teams and we will still provide liaison and advice at a national policy level and communicate any messages through when necessary. We will also continue to work with local Healthwatch HWB representatives through our Care and Health Improvement Programme over the coming year.
If you are continuing to commission local Healthwatch in your area then please make sure you are signed up to the Knowledge Hub where you can access 3 years of archived discussion and support material. We have also kept a Healthwatch page as part of the LGA si with up-to-date documents for those new to Healthwatch commissioning.
Local Healthwatch: Progress and Promise' – As you know, the Department of Health commissioned the King's Fund to look at the impact and effectiveness of local Healthwatch since they were set up in April 2013. The report has now been published and you can read it on GOV.UK. I've also put a copy up on the Knowledge Hub.
One of the findings in the report is around the important role local authority commissioners play in the development and overall effectiveness of their local Healthwatch and there are some recommendations about how this might be developed going forward. Colleagues at DH have asked me to pass on their thanks to everyone who took part.
- The Knowledge Hub: if you hand over your commissioning responsibilities of Healthwatch to another officer at any point please pass on the link to the Healthwatch commissioning group so they have access to all of our documentation and conversations. Also don't forget the group is closed for commissioners only so do use it to ask any questions/search for good practice in between commissioner meetings.
- Regional Commissioners' Meetings: the LGA will no longer be booking rooms or facilitating Healthwatch commissioners' meetings on a quarterly basis for your regional groups. To help groups self-facilitate meetings I've uploaded a commissioner contact sheet to our private group on the knowledge hub which is as up-to-date as possible and includes contact details for colleagues at Healthwatch England from their regional teams.
- Local Healthwatch Governance: as some of you are aware we have been updating our guidance materials for local Healthwatch governance. There have been some delays with this piece of work and it will now be published in April. I'll send this out by email when it is complete as well as putting it on the LGA Healthwatch site and uploading onto the Knowledge Hub.
We hope you have found the support and materials from the LGA over the past few years helpful and encourage you all to stay connected to offer peer support and share learning through network meetings and on the Knowledge Hub.
John Tench
Healthwatch Adviser
john.tench@local.gov.uk
07786 541890
REVISED CODE OF PRACTICE: MENTAL HEALTH ACT (1983) COMING INTO EFFECT ON 01 APRIL 2015
The Revised Mental Health Code of Practice comes into effect from the 1 April 2015. The Care Quality Commission was one of a number of stakeholders who contributed to the development of the Revised Code of Practice. The Department of Health has published a new reference guide and impact assessment to accompany the Code.
The revised Code seeks to provide stronger protection for patients and clarify roles, rights and responsibilities. This includes involving the patient and as appropriate, their families and carers in discussions about the patient’s care at every stage; providing personalised care; minimising the use of inappropriate blanket restrictions, restrictive interventions and the use of police cells as places of safety.
The key changes include 5 new guiding principles;
information to be provided to victims of part 3 patients;
appropriately applied;
- The news story from 15 January 2015 can be viewed here:
https://www.gov.uk/government/news/new-mental-health-act-code-of-practice
- The Code is available electronically at:
www.gov.uk/government/publications/code-of-practice-mental-health-act-1983
- Hard copies are available to order from this site or directly from the Government Stationary Office:
http://www.tsoshop.co.uk/bookstore.asp?FO=1160007&DI=642031
- Supporting documentation, including the Consultation response, Equality Analysis and Impact Assessment is available at:
https://www.gov.uk/government/consultations/changes-to-mental-health-act-1983-code-of-practice
- A revised Reference Guide to the Mental Health Act is available at:
https://www.gov.uk/government/publications/mental-health-act-1983-reference-guide
Please also see the link below for the consultation No voice unheard, no right ignored – a consultation for people with learning disabilities, autism and mental health conditions. The document seeks to explores views on a number of issues related to supporting people with learning disability, autism and mental health conditions. This includes some relating to the Mental Health Act which were raised during the recent consultation on the revised Mental Health Act Code of Practice. The consultation started on 6 March and ends on the 29 May 2015:
https://www.gov.uk/government/consultations/strengthening-rights-for-people-with-learning-disabilities
The Revised Mental Health Code of Practice comes into effect from the 1 April 2015. The Care Quality Commission was one of a number of stakeholders who contributed to the development of the Revised Code of Practice. The Department of Health has published a new reference guide and impact assessment to accompany the Code.
The revised Code seeks to provide stronger protection for patients and clarify roles, rights and responsibilities. This includes involving the patient and as appropriate, their families and carers in discussions about the patient’s care at every stage; providing personalised care; minimising the use of inappropriate blanket restrictions, restrictive interventions and the use of police cells as places of safety.
The key changes include 5 new guiding principles;
- New chapters on care planning, human rights, equality and health inequalities, consideration of when to use the
information to be provided to victims of part 3 patients;
- New sections on physical healthcare, blanket restrictions, duties under section 140, to support patients with
appropriately applied;
- Significantly updated chapters on the appropriate use of restrictive interventions, including particularly seclusion and long-term
- Segregation, police powers and places of safety and in relation to decisions about whether to discharge or not; and
- Further guidance on how to support children and young people, those with a learning disability or autism, and in relation to part 3 patients.
- The news story from 15 January 2015 can be viewed here:
https://www.gov.uk/government/news/new-mental-health-act-code-of-practice
- The Code is available electronically at:
www.gov.uk/government/publications/code-of-practice-mental-health-act-1983
- Hard copies are available to order from this site or directly from the Government Stationary Office:
http://www.tsoshop.co.uk/bookstore.asp?FO=1160007&DI=642031
- Supporting documentation, including the Consultation response, Equality Analysis and Impact Assessment is available at:
https://www.gov.uk/government/consultations/changes-to-mental-health-act-1983-code-of-practice
- A revised Reference Guide to the Mental Health Act is available at:
https://www.gov.uk/government/publications/mental-health-act-1983-reference-guide
Please also see the link below for the consultation No voice unheard, no right ignored – a consultation for people with learning disabilities, autism and mental health conditions. The document seeks to explores views on a number of issues related to supporting people with learning disability, autism and mental health conditions. This includes some relating to the Mental Health Act which were raised during the recent consultation on the revised Mental Health Act Code of Practice. The consultation started on 6 March and ends on the 29 May 2015:
https://www.gov.uk/government/consultations/strengthening-rights-for-people-with-learning-disabilities
CQC DELAYS INSPECTION OF GPs
The CQC has extended its deadline for inspecting and rating all GP Practices by six months because it does not have the staff to hit its original April 2016 target, the watchdog's Chief Executive has admitted. The CQC has now pledged to visit, inspect and rate all Practices by 30 September 2016 - a six-month extension from its previous plans to get this completed by the end of March. The extension means the CQC will now have two years overall from when the scheme was launched in October 2014 to inspect the 8,000 Practices in England.
Its Chief Executive, David Behan, said there were a ‘number of reasons’ for pushing the date back, but a key limiting factor was that it had failed to recruit sufficient Lead Inspectors to meet the April target, which would have required the CQC to get through over 100 inspections a week.
A third short of inspectors
Practice inspection teams are made up of five people - a Lead Inspector employed by the CQC, a Lay Inspector and Specialist Advisors – including at least one GP. To date the CQC has only managed to recruit 148 Lead Inspectors, when it required 222 to meet its ambitious targets, meaning it is 74 (33%) short.
The CQC has extended its deadline for inspecting and rating all GP Practices by six months because it does not have the staff to hit its original April 2016 target, the watchdog's Chief Executive has admitted. The CQC has now pledged to visit, inspect and rate all Practices by 30 September 2016 - a six-month extension from its previous plans to get this completed by the end of March. The extension means the CQC will now have two years overall from when the scheme was launched in October 2014 to inspect the 8,000 Practices in England.
Its Chief Executive, David Behan, said there were a ‘number of reasons’ for pushing the date back, but a key limiting factor was that it had failed to recruit sufficient Lead Inspectors to meet the April target, which would have required the CQC to get through over 100 inspections a week.
A third short of inspectors
Practice inspection teams are made up of five people - a Lead Inspector employed by the CQC, a Lay Inspector and Specialist Advisors – including at least one GP. To date the CQC has only managed to recruit 148 Lead Inspectors, when it required 222 to meet its ambitious targets, meaning it is 74 (33%) short.
CODE OF PRACTICE ON CONSULTATION and CONSULTATION PRINCIPLES
Click on the images to download ...
Click on the images to download ...
|
Ongoing dialogue between Government and stakeholders is an important part of policymaking. This dialogue will, at times, need to become more formal and more public. When developing a new policy or considering a change to existing policies, processes or practices, it will often be desirable to carry out a formal, time-bound, public, written consultation exercise. This kind of exercise should be open to anyone to respond but should be designed to seek views from those who would be affected by, or those who have a particular interest in, the new policy or change in policy. Formal consultation exercises can expose to scrutiny the Government’s preliminary policy analysis and the policy or implementation options under consideration.
|
COMPLAINT TO NHSE ABOUT HEALTHCARE IN DETENTION CENTRES
Failure to Involve Patients and the Public in the Commissioning of Immigration Detainee Healthcare
Letter To: Kate Davies, Head of Public Health, Armed Forces Health and Offender Health
From: Christine Hogg, Chair, Medical Justice - and Malcolm Alexander, Chair, HAPIA
Failure to Involve Patients and the Public in the Commissioning of Immigration Detainee Healthcare
Letter To: Kate Davies, Head of Public Health, Armed Forces Health and Offender Health
From: Christine Hogg, Chair, Medical Justice - and Malcolm Alexander, Chair, HAPIA
CARE CERTIFICATE
Lord Taylor of Warwick Non-affiliated 6th March 2015
To ask Her Majesty’s Government what steps they are taking to improve training and development in the care sector.
It is the responsibility of individual employers to ensure that staff are appropriately trained and competent to carry out the roles they are employed to provide. The Department continues to work with Skills for Care to develop a comprehensive suite of standards and qualifications to support employers in developing the care sector workforce.
From 1 April 2015, the Department is introducing the Care Certificate for new healthcare assistants and social care support workers to enable them to receive the high quality and consistent training and support they need to do their jobs.
Lord Taylor of Warwick Non-affiliated 6th March 2015
To ask Her Majesty’s Government what steps they are taking to improve training and development in the care sector.
- Hansard source (Citation: HL Deb, 6 March 2015, cW)
It is the responsibility of individual employers to ensure that staff are appropriately trained and competent to carry out the roles they are employed to provide. The Department continues to work with Skills for Care to develop a comprehensive suite of standards and qualifications to support employers in developing the care sector workforce.
From 1 April 2015, the Department is introducing the Care Certificate for new healthcare assistants and social care support workers to enable them to receive the high quality and consistent training and support they need to do their jobs.
JOINT COMMISSIONING CCGs
A third of CCGs have been approved to jointly commission primary care with NHS England as part of plans to develop co-commissioning.
The 87 GP-led groups will share commissioning functions with NHS England from April. The announcement means over 70% of CCGs will take on greater commissioning responsibilities [after the 64 CCGs which will take fully delegated control of commissioning were announced last month.]
CCGs taking on joint commissioning will share control over managing contracts, designing PMS and APMS deals, contractual action such as remedial notices and removing contracts, enhanced services and local QOF alternatives. They will be able, jointly with NHS England, to establish new practices, approve mergers and award discretionary payments.
Click here to download the list of CCGs ...
A third of CCGs have been approved to jointly commission primary care with NHS England as part of plans to develop co-commissioning.
The 87 GP-led groups will share commissioning functions with NHS England from April. The announcement means over 70% of CCGs will take on greater commissioning responsibilities [after the 64 CCGs which will take fully delegated control of commissioning were announced last month.]
CCGs taking on joint commissioning will share control over managing contracts, designing PMS and APMS deals, contractual action such as remedial notices and removing contracts, enhanced services and local QOF alternatives. They will be able, jointly with NHS England, to establish new practices, approve mergers and award discretionary payments.
Click here to download the list of CCGs ...
ENTRY TO PREMISES BY LOCAL HEALTHWATCH REPRESENTATIVES
Upcoming business - Tuesday, 10 March 2015
Lords: Grand Committee
Draft Local Authorities (Public Health Functions and Entry to Premises by Local Healthwatch Representatives) and Local Authority (Public Health, Health and Wellbeing Boards and Health Scrutiny) (Amendment) Regulations 2015 Orders and Regulations
Upcoming business - Tuesday, 10 March 2015
Lords: Grand Committee
Draft Local Authorities (Public Health Functions and Entry to Premises by Local Healthwatch Representatives) and Local Authority (Public Health, Health and Wellbeing Boards and Health Scrutiny) (Amendment) Regulations 2015 Orders and Regulations
RESHAPING PRIMARY CARE - AN OPPORTUNITY TO BE INVOLVED (All the places have now been filled)
An opportunity has arisen to help shape primary care development in England. A workshop is being held in central London on Monday 23rd March from 10:30 to 16:00 to look at what matters most to patients and carers in primary care. The workshop will form the first part of an extensive engagement and consultation process that will feed into the development of a framework for patients and carers expectations in primary care. Attendees will be made up of key professionals within primary care as well as an extensive number of patients and carers.
We are therefore looking for a number of patient and carer representatives who have experience of giving their views on primary care, e.g. involved in local GP Patient Participation Groups. We will provide lunch and reimburse expenses e.g. travel. If you are interested in being part of the workshop, please complete the attached form by the 6th March and email back to lynda.norton@nhs.net. You can also call Lynda on 0113 825 1108 for further information about the workshop or if you have any questions/queries.
An opportunity has arisen to help shape primary care development in England. A workshop is being held in central London on Monday 23rd March from 10:30 to 16:00 to look at what matters most to patients and carers in primary care. The workshop will form the first part of an extensive engagement and consultation process that will feed into the development of a framework for patients and carers expectations in primary care. Attendees will be made up of key professionals within primary care as well as an extensive number of patients and carers.
We are therefore looking for a number of patient and carer representatives who have experience of giving their views on primary care, e.g. involved in local GP Patient Participation Groups. We will provide lunch and reimburse expenses e.g. travel. If you are interested in being part of the workshop, please complete the attached form by the 6th March and email back to lynda.norton@nhs.net. You can also call Lynda on 0113 825 1108 for further information about the workshop or if you have any questions/queries.